The role of fructose in the development of gout
07/03/2018 OxiPur
Uric acid and its salts, known as urates, are an end-product of the metabolism that is excreted with the urine. Unfortunately, urates are poorly soluble in water. In contrast to other mammals, humans don't have the enzymes to convert them into more soluble compounds. Therefore, the human uric acid level of 6.4 mg/dl is very high in comparison – it is just below the physical solubility limit. In some cases this can have negative consequences: If the uric acid concentration rises above this level, urate crystals precipitate and the long-lasting exposure may inflict damage on the body. In the long term, an elevated value of 7.0 mg/dl and above is considered a risk factor for the development of gout.

There are several factors that affect the serum uric acid levels. Although gout disease has been known for centuries, the impact of the diet has not yet been fully understood. The largest proportion of the urate load comes from the metabolism itself (see figure 1). The body constantly replaces damaged tissues and dead cells and the breakdown of their proteins leads to the formation of significant amounts of uric acid.
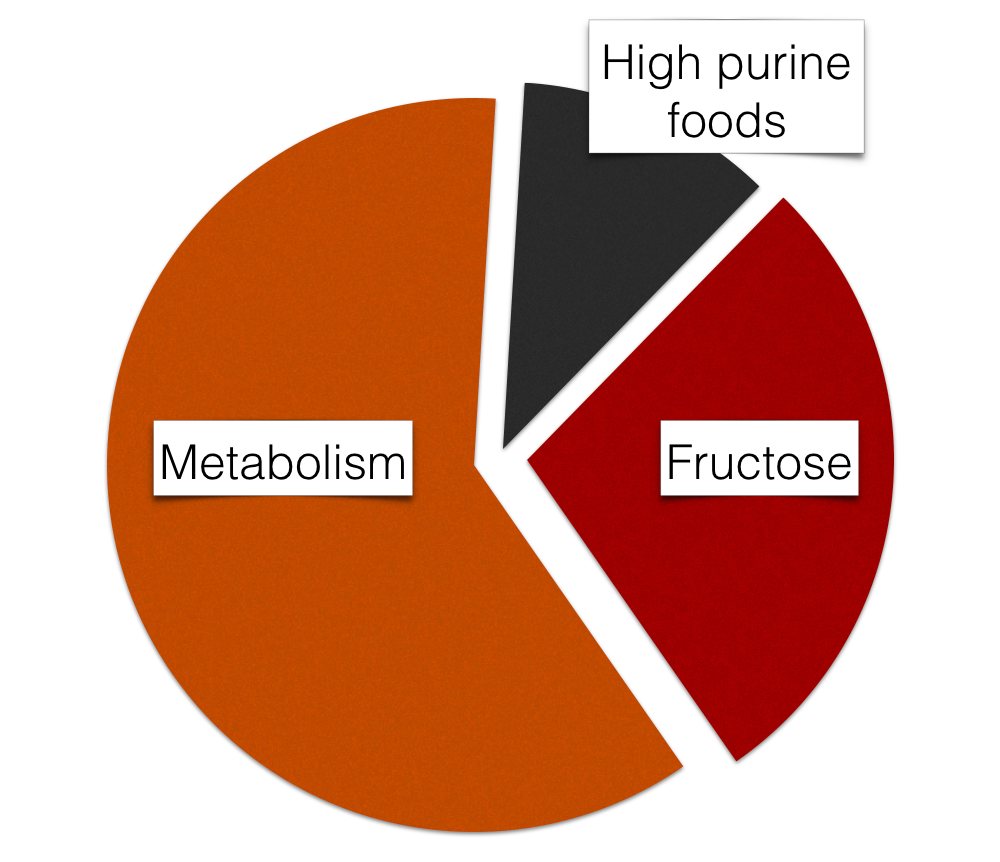 ▲ Figure 1: Impact of different factors on the uric acid level.
▲ Figure 1: Impact of different factors on the uric acid level.
A diet rich in purines also increases the serum uric acid levels. However, dietary purines only make up about 1–2 mg/dl – a rather small proportion of the total load. Exogenous dietary purines play a significantly smaller role than has been thought for a long time. For this reason, the one-sided focus on dietary purines alone proved insufficient to manage gout. That does not mean that reducing the purine intake is unnecessary; a low purine diet is still a cornerstone of the dietary therapy of hyperuricemia and gout.
Studies have shown that the majority of gout sufferers are overproducing uric acid – and that the main driver of this overproduction might be the excessive intake of fructose. It is more than likely that everbody overproduces uric acid when the fructose intake exceeds a critical amount.
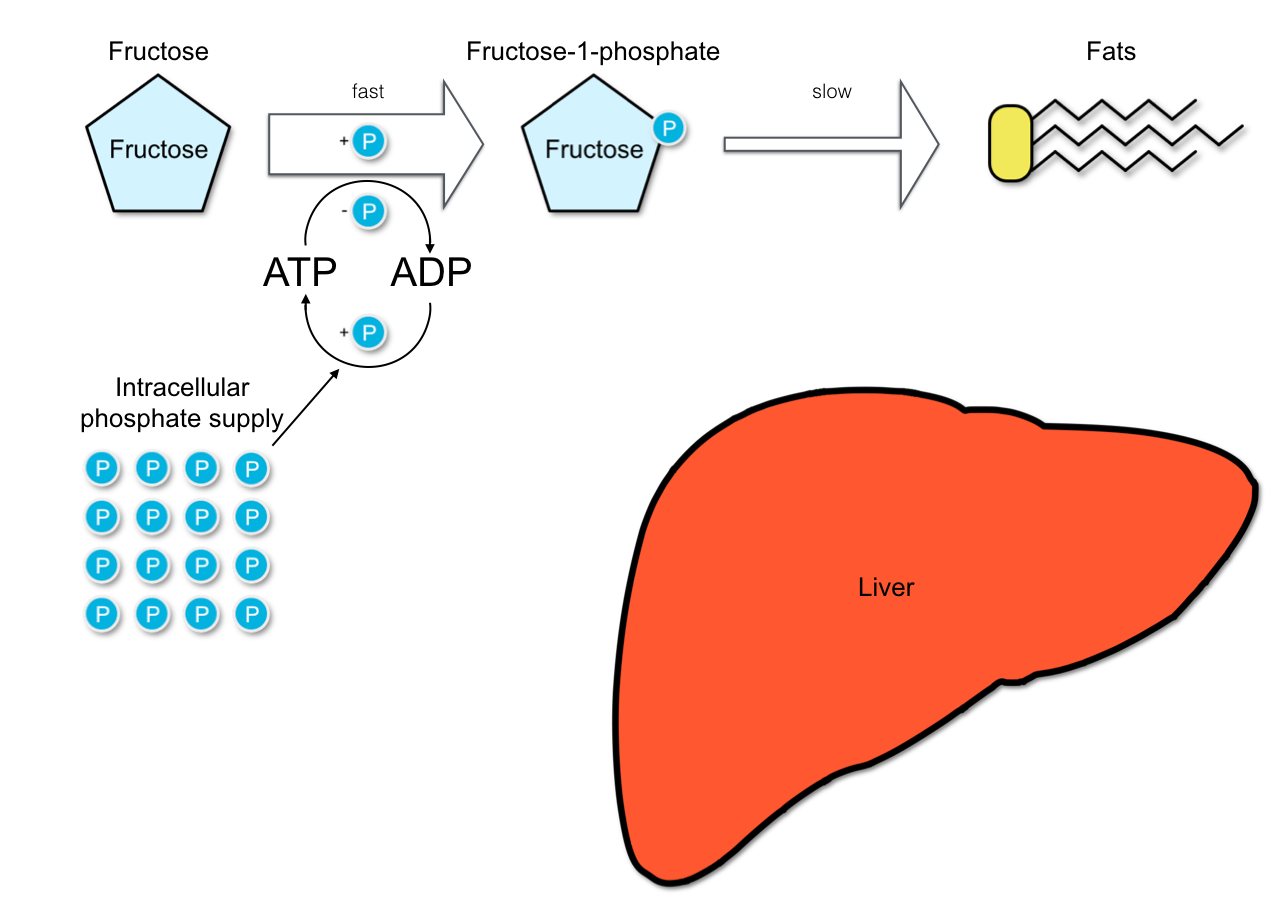
▲ Figure 2: Fructose metabolism in the liver.
Fructose is primarily metabolized in the liver. In the course of different reaction steps it is converted into triglycerides, major constituents of the body fat (see figure 2). The individual chemical reactions take place at different speeds: The first step, the phosphorylation of fructose, is very fast, while the second step, the enzymatic cleavage of fructose-1-phosphate, is very slow.
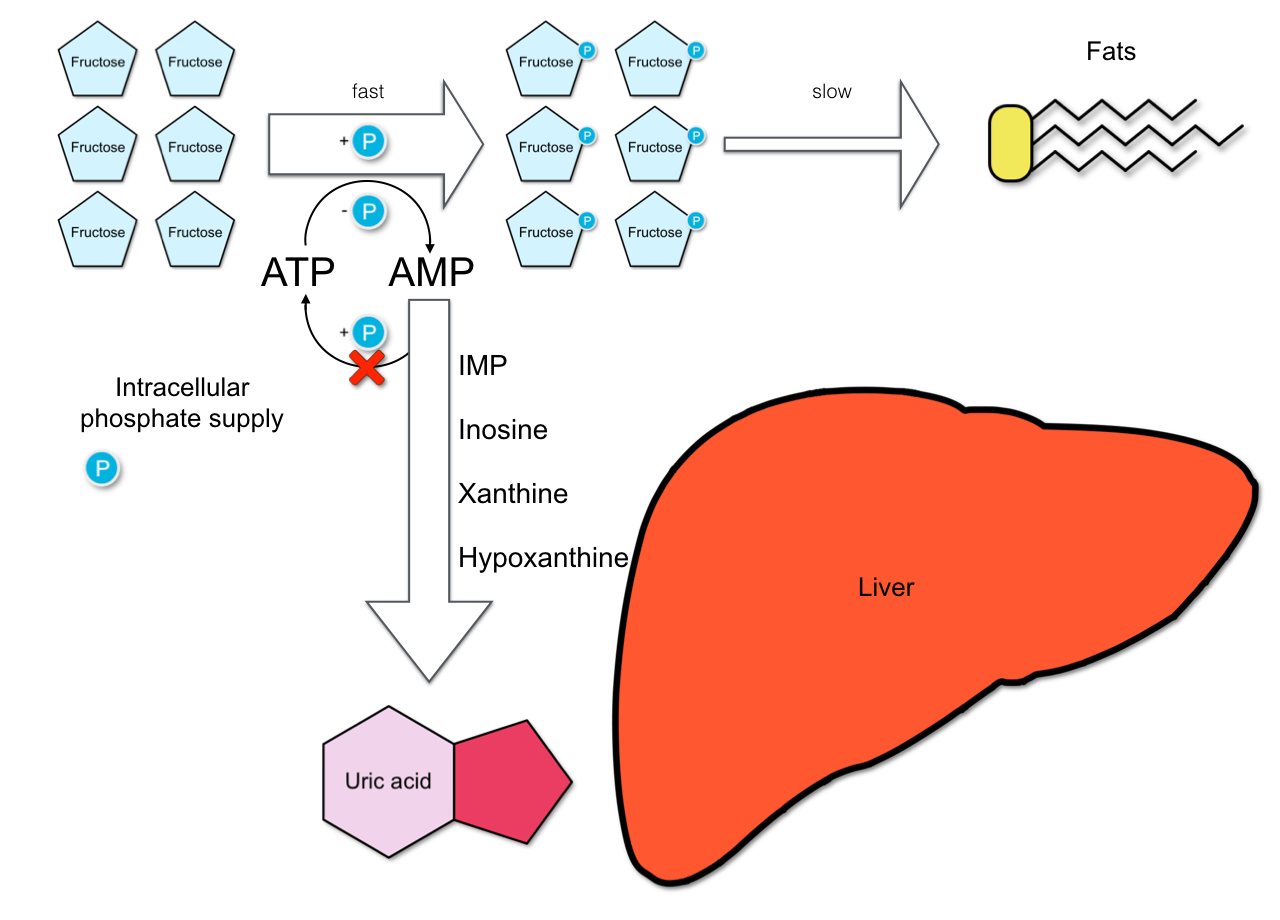
▲ Figure 3: Fructose metabolism of large quantities of fructose.
When the liver is flooded with a huge quantity of fructose this can result in the depletion of intracellular phosphate reservoirs, inhibiting the regeneration of adenosine triphosphate (ATP) (see figure 3). As a consequence of the phosphate deficit, adenosine monophosphate (AMP) and adenosine diphosphate (ADP) accumulate in the system and are then catabolyzed into uric acid.
So a diet rich in fructose is not per se problematic for gout sufferers – the human organism is capable of digesting moderate amounts of fructose without consequences. However, when the liver is flooded with large quantities of fructose in a short period of time, it is forced into a biochemical pathway that enables the formation of uric acid and can cause hyperuricemia.
Back to blog
References:
E. Kedar et al., A Perspective on Diet and Gout, Advances in Chronic Kidney Disease 19:6 (2012), 392–397
R. Johnson et al., Sugar, Uric Acid, and the Etiology of Diabetes and Obesity, Diabetes 62 (2013), 3307–3315
E. Prado de Oliveira et al., High plasma uric acid concentration: causes and consequences, Diabetology & Metabolic Snydrome 4 (2012), 1–7
J. Villa-Rodriguez et al., Green and Chamomile Teas, but not Acarbose, Attenuate Glucose and Fructose Transport via Inhibition of GLUT2 and GLUT5, Mol. Nutr. Food Res. 61 (2017), 1700566, 1-14

What factors can influence the uric acid level?
There are several factors that affect the serum uric acid levels. Although gout disease has been known for centuries, the impact of the diet has not yet been fully understood. The largest proportion of the urate load comes from the metabolism itself (see figure 1). The body constantly replaces damaged tissues and dead cells and the breakdown of their proteins leads to the formation of significant amounts of uric acid.

A diet rich in purines also increases the serum uric acid levels. However, dietary purines only make up about 1–2 mg/dl – a rather small proportion of the total load. Exogenous dietary purines play a significantly smaller role than has been thought for a long time. For this reason, the one-sided focus on dietary purines alone proved insufficient to manage gout. That does not mean that reducing the purine intake is unnecessary; a low purine diet is still a cornerstone of the dietary therapy of hyperuricemia and gout.
Uric acid overproduction
Studies have shown that the majority of gout sufferers are overproducing uric acid – and that the main driver of this overproduction might be the excessive intake of fructose. It is more than likely that everbody overproduces uric acid when the fructose intake exceeds a critical amount.

▲ Figure 2: Fructose metabolism in the liver.
Fructose is primarily metabolized in the liver. In the course of different reaction steps it is converted into triglycerides, major constituents of the body fat (see figure 2). The individual chemical reactions take place at different speeds: The first step, the phosphorylation of fructose, is very fast, while the second step, the enzymatic cleavage of fructose-1-phosphate, is very slow.

▲ Figure 3: Fructose metabolism of large quantities of fructose.
When the liver is flooded with a huge quantity of fructose this can result in the depletion of intracellular phosphate reservoirs, inhibiting the regeneration of adenosine triphosphate (ATP) (see figure 3). As a consequence of the phosphate deficit, adenosine monophosphate (AMP) and adenosine diphosphate (ADP) accumulate in the system and are then catabolyzed into uric acid.
So a diet rich in fructose is not per se problematic for gout sufferers – the human organism is capable of digesting moderate amounts of fructose without consequences. However, when the liver is flooded with large quantities of fructose in a short period of time, it is forced into a biochemical pathway that enables the formation of uric acid and can cause hyperuricemia.
Why do we care so much about this topic?
 We have been developing our "OxiPur" app about gout and oxalates for many years and are happy to share our knowledge with you. Check it out:
We have been developing our "OxiPur" app about gout and oxalates for many years and are happy to share our knowledge with you. Check it out:
Share article
Share article
Back to blog
References:
E. Kedar et al., A Perspective on Diet and Gout, Advances in Chronic Kidney Disease 19:6 (2012), 392–397
R. Johnson et al., Sugar, Uric Acid, and the Etiology of Diabetes and Obesity, Diabetes 62 (2013), 3307–3315
E. Prado de Oliveira et al., High plasma uric acid concentration: causes and consequences, Diabetology & Metabolic Snydrome 4 (2012), 1–7
J. Villa-Rodriguez et al., Green and Chamomile Teas, but not Acarbose, Attenuate Glucose and Fructose Transport via Inhibition of GLUT2 and GLUT5, Mol. Nutr. Food Res. 61 (2017), 1700566, 1-14
![[Blog]](../../rw_common/images/baliza_logo_retina.png)
